What is postpartum depression?
Postpartum depression is an emotional reaction that may begin a few days or months after delivery and usually doesn’t last longer than two weeks. Mothers and fathers may feel irritable, anxious, tired and moody. It may be difficult to sleep for those with postpartum depression. Sometimes this depression develops into postpartum anxiety, which lasts longer and is characterized by intensified postpartum depression symptoms. If you don’t treat this depression it may harm the development of your baby. Parents with postpartum depression make less eye contact and smile less. This may affect the baby’s forming of attachment to the mother and father.
At Barends Psychology Practice, we treat depression Online and in person. Book your first free of charge session now. Go to Contact us. (Depending on your health insurance, treatment may be reimbursed).
Quick Jump-to menu:
Postpartum depression in women.
Up to 80% of the mothers experience feeling a bit depressed for a couple of weeks, the baby blues. They are moody, irritable, anxious, they cry a bit more and they might have sleeping problems. Usually these depressed feelings fade away with some rest and some help with the baby. However, if these feelings are still present after a few weeks, you might have postpartum depression. If left untreated, postpartum depression may interfere with mother-child bonding and can cause family problems. Children of mothers with untreated postpartum depression have a bigger chance of developing sleeping problems, behavioural problems (problems with feeding, being hyperactive and temper tantrums). Language development may be delayed as well. Postpartum depression may last a few weeks, but could easily last up to a year.
Postpartum depression in men.
Between 4 and 25% of the fathers develop paternal postnatal depression in the first two months after delivery.* Hormonal changes (testosterone level, but also cortisol, estrogen and vasopressin) may be biological risk factors for developing postpartum depression. There is a bigger chance of developing postpartum depression if your partner has it too. Fathers with postpartum depression cause more marital problems and may also affect the development of the baby (and other children). They usually make less eye contact and smile less as fathers who are not depressed. The bigger the disengagement, the bigger the risk that the baby will have trouble forming close attachments. Babies and children may develop behavioural and emotional problems. Risk factors for fathers are: being a dad of twins, feeling depressed or anxious during pregnancy, having a baby with sleeping problems or having a baby who cries a lot. It is very important for fathers to be screened on postpartum depression and if needed treated.
*Between 4 and 25%: this huge difference is explained by the different questionnaires and others measuring tools used in various studies.
(Advertisement. For more information, please scroll down.)
Postpartum depression – symptoms.
At any moment during the first year after giving birth you might develop postnatal depression. Postnatal depression usually starts within the first two months after giving birth. Postpartum depression can also occur in women who suffered a miscarriage. In the beginning postpartum depression looks like the baby blues. But over time the signs and symptoms last longer and become more intense. This can result in experiencing difficulty to take care of your baby. The symptoms may include:
- Depressed mood.
- Sleeping problems.
- Having the feeling that you’re a bad parent.
- Loss of energy or overwhelming fatigue.
- Low-self esteem, feeling worthless, inadequate or ashamed.
- Intense irritability and anger.
- Lack of joy in life.
- Decreased appetite for sex.
- Difficulty bonding with your baby.
- Difficulty focusing, concentrating or being forgetful.
- Thoughts of harming yourself or the baby.
- Loss of appetite.
- Severe anxiety and worry.
- Excessive crying.
Please be aware that many women may experience one or more symptoms of postpartum depression, but never develop it.
Postpartum depression – risks.
You are more at risk of developing postpartum depression if:
- There is a history of depression or anxiety running in the family.
- You suffer from depression or anxiety during pregnancy.
- You have a none supportive partner.
- You have financial problems.
- You have marital problems, or just went through divorce.
- The pregnancy was not planned.
- You experience(d) a major life event (losing a job, moving to a different town, losing a relative).
- You experienced childhood trauma, were victim of abuse or have a dysfunctional family.
Please be aware that these risk factors do not cause postnatal depression but may contribute to its development. Some women develop postpartum depression without having any of the above mentioned risk factors, while others with several may not develop postpartum depression at all.
Postpartum depression – causes.
(Advertisement. For more information, please scroll down.)
Most likely a combination of factors contribute to the development of postnatal depression. A brief overview:
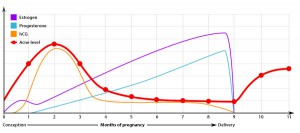
- Hormones – After delivery the hormones estrogen and progesterone drop dramatically, together with the hormones produced by the thyroid gland. Hormonal imbalance can have a drastic effect on people. Due to the drop in hormones someone may be feeling depressed, tired and lack energy.
- Emotional – Right after delivery women experience an emotional high, but this disappears as quickly as it came. This feeling may be replaced by many new responsibilities that come with parenthood. Taking care of a newborn can be tiring, frustrating, frightening and may drain your energy. This can result in feeling depressed and insecure. It may make you cry more, decrease your sex drive, appetite and make it difficult for you to enjoy life.
- Lifestyle changes – All of a sudden the baby is your top priority. There is little time to socialize, to go out for dinner or go shopping. Wearing fancy clothes may be a decision you regret when your newborn spills some milk. Your baby may be a difficult baby (think of reflux, being lactose intolerant, problems breast feeding etc.).
Postpartum depression – prevention / treatment.
If you think you have postnatal depression then please make an appointment with your therapist or contact Barends Psychology Practice for online therapy so we can either treat you or guide you through this difficult time. Here are some other helpful tips:
- Make sure you have a routine for both your baby and yourself. Do not forget to make space for little breaks and rest enough.
- Talk with your partner about the household responsibilities and who takes care of the baby at night, who burps the baby etc..
- Ask for help with certain house holding tasks or other stuff like groceries shopping. You can turn to your friends or family. Do not underestimate the impact a newborn may have on your daily routine.
- Talk to your partner, friends, family and therapist about your fears and difficulties. Talking about your feelings can be a major stress relief.
Literature.
- [1] Robertson, E., Grace, S., Wallington, T., & Stewart, D. E., 2004. Antenatal risk factors for postpartum depression: a synthesis of recent literature. General Hospital Psych., 26, 289-295.
- [2] Grace, S. L., Evindar, A., Stewart. D. E., 2003. The effect of postpartum depression on child cognitive development and behaviour: a review and critical analysis of the literature. Arch Womens Ment Health, 6, 263-274.
Quick Jump-to menu:
- What is depression?
- Depression causes.
- Diagnosing depression.
- Depression treatment.
- Interesting depression facts.
- Mental Disorders main page.
- Back to the homepage.