Caffeine and mental disorders – Barends Psychology Practice
Little is known about the interaction between caffeine and mental disorders. Almost every mental health clinic serves caffeine holding drinks to its clients and employees. Does this suggest that caffeine and mental disorders make a good match? Caffeine is famous for its stimulating effect and for its social aspect. Other positive effects are an increase in metabolism, reduced risk of Parkinson’s Disease, increased levels of neurotransmitters like serotonin, dopamine, and epinephrine. Negative effects: it can increase blood pressure, reduce control of fine movements, contributes to increased insomnia and sleep latency, and caffeine is Addictive! Do these positive and negative side effects affect the interaction between caffeine and mental disorders?
In some cases caffeine and mental disorders are an accepted combination: some people with ADHD use caffeine because of its stimulating effect. And sometimes caffeine can take the edge of a mild depression. Also caffeine and mental disorders tend to go perfectly well together when the person does not consume caffeine regularly. On the other hand caffeine consumption can make people more anxious. Let’s take a closer look at the interaction between caffeine and mental disorders.
At Barends Psychology Practice, we offer (online) therapy for all kinds of mental disorders. Contact us to schedule a first, free of charge, online session. (Depending on your health insurance, sometimes treatment can be reimbursed).
Quick Jump-to menu:
- General caffeine information.
- Caffeine and anxiety.
- Caffeine and panic attacks.
- Caffeine and PTSD.
- Caffeine and depression.
- Caffeine and schizophrenia.
- Literature.
General caffeine information.
Caffeine comes from coffee beans or can be made in the laboratory. You can find caffeine in coffee, tea, soda, energy drinks, pills, yerba mate, kola nut, cacao and cocoa. It is estimated that the global consumption of caffeine reaches 120.000 tonnes per year (Wikipedia). 87% of the Americans consume caffeine. In Scandinavia, Germany, and The Netherlands even more people consume caffeine [2].
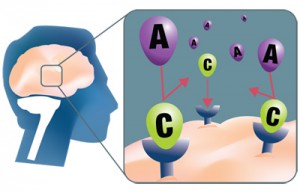
Caffeine makes sure you don’t get sleepy by blocking the reception of a chemical (adenosine) in the brain. This makes you feel more alert and awake. However, this effect does not last. Regular caffeine usage causes your body to get used to caffeine. Your body responds less to its stimulating effect, unless you take more caffeine. Eventually, probably the only effect caffeine has on you is its anti-sleep effect.
There is a difference between those who consume caffeine regularly and those who consume caffeine once in a while. For instance, regular caffeine users usually do not experience an increased heart beat after consuming caffeine, whereas the people who consume caffeine only once in a while do experience an increase in heart beat. The latter group also feel the urge to move around more (tapping feet or twitching), whereas the regular users do not experience this effect. It is up to you to decide whether or not caffeine affects you.
(Advertisement. For more information, please scroll down.)
Caffeine and mental disorders – Anxiety.
In general, people with Generalized Anxiety Disorder (GAD) are more sensitive to caffeine consumption than people without GAD [1]. This increased sensitivity causes some people with anxiety disorders to perceive physical symptoms (e.g. increased pulse) more intense. In other words this increased sensitivity causes more anxiety in some people with anxiety disorder. For treatment this increased sensitivity could be troublesome, because of the perceived increased anxiety. So the interaction between caffeine and mental disorders in the anxiety range can be harmful for treatment.
Caffeine and mental disorders – Panic Attacks.
People who have panic attacks are most likely increased sensitive to changes in their body. Panic attacks are triggered when a person experiences different physical sensations. Caffeine consumption can make people with panic attacks perceive physical changes as if they are actual panic attack symptoms. This happens more automatic than conscious, so it is difficult to notice.
For example:
- Increased heart rate – Caffeine can increase heart rate (this effect is less likely to occur in regular caffeine consumers). This increase in heart rate can be noticed by those with panic attacks and makes them panic, resulting in a panic attack.
- Stomach discomfort – Caffeine can produce a discomforting feeling in the stomach (e.g. aches and pains). These feelings of discomfort can trigger panic attacks in the same way as with increased heart rate.
Caffeine and mental disorders – Post-traumatic Stress disorder.
At the moment there is no hard evidence of caffeine inducing Post-traumatic Stress Disorder symptoms. But more research is needed. However, there is some circumstantial evidence that suggests that caffeine affects some of its symptoms. According to Lane et al. [4] 3,5mg/kg caffeine (roughly 3,5 cups of coffee) is enough to enhance the adrenaline release by 233% in regular caffeine consumers and the ones who occasionally consume caffeine. Also caffeine can trigger anxiety in people. Both adrenaline and anxiety are symptoms that can be Post-traumatic stress disorder related. Together with the fact that caffeine can disturb your sleep, it is easy to make the connection between caffeine and mental disorders when it comes to PTSD.
(Advertisement. For more information, please scroll down.)
Caffeine and mental disorders – Major Depressive Disorder.
There is no direct clear link between caffeine consumption and depression, but there is some indirect evidence suggesting that caffeine may worsen depression. Especially people who are sensitive to the effect of caffeine or those who consumed too much caffeine. Caffeine may cause sleeping problems: falling asleep and staying asleep. Sleeping problems are associated with depression. The sleeping problems make depressed people more tired during the day, making it more difficult for them to become active. Being active is an important step to get out of depression. However, if you are depressed: do not quit caffeine consumption at once, because it can worsen depression due to its withdrawal symptoms.
note: consuming caffeine has been associated with reducing risks of becoming depressed [5], while there is no link between caffeine consumption and the response to antidepressants [6].
Caffeine and mental disorders – Schizophrenia.
People with schizophrenia have higher caffeine consumption than other people. The reasons are unclear. Unlike the popular idea that caffeine and mental disorders go hand in hand, research shows that removing caffeine from people with schizophrenia does not affect the positive or negative symptoms of schizophrenia [3]. However consuming high doses of caffeine may induce psychosis (this effect might not be present with those who are regular caffeine consumers).
Caffeine and mental disorders – Literature.
-
[1] Bruce, M.; Scott, N.; Shine, P., and Lader, M., 1992. Anxiogenic effects of caffeine in patients with anxiety disorders. Arch Gen Psychiatry, 49, 867-869.
[2] Heishman S.J., Henningfield J.E. (1992). Stimulus functions of caffeine in humans: relation to dependence potential. Neurosci Biobehav Rev., 16, 273-287.
[3] Hughes, J. R., McHugh, P., and Holtzman, S. (1998). Alcohol and drug abuse: Caffeine and Schizophrenia. Psychiatric Services, 49, 1415-1417.
[4] Lane J.D., Adcock, R. A., Williams, R. B., & Kuhn, C. M. (1990). Caffeine effects on cardiovascular and neuroendocrine responses to acute psychosocial stress and their relationship to level of habitual caffeine consumption. Psychosom Med. 52, 320-336.
[5] Smith, A. P., 2009. Caffeine, cognitive failures and health in a non-working community sample. Hum Psychofarmacol, 24, 29-34.
[6] Worthington, J., Fava M., Agustin C., Alpert J., Nierenberg A. A., Pava J. A. et al. (1996). Consumption of alcohol, nicotine, and caffeine among depressed outpatients: relationship with response to treatment. Psychosomatics, 37, 518-522.